Hennepin Healthcare Research Institute (HHRI)
How systemic barriers and social drivers impact health more than other factors
Photo: Adobe Stock Image
GOAL: The Health, Homelessness, & Criminal Justice (HHCJ) Lab is nestled within one of the largest medical research nonprofits in Minnesota, Hennepin Healthcare Research Institute (HHRI), which is connected to the Hennepin Healthcare System (HHS). HHCJ's research focuses on Social Determinants of Health (SDOH) and how these factor into people's overall well-being, however, not everyone is born with the same privileges or advantages.
The Health, Homelessness, & Criminal Justice (HHCJ) Lab is nestled within one of the largest medical research nonprofits in Minnesota, Hennepin Healthcare Research Institute (HHRI), which is connected to the Hennepin Healthcare System (HHS). HHCJ’s vision is “Thriving communities without health inequities driven by homelessness or criminal justice involvement.” This is based on robust evidence that these and other social drivers have much more impact on health than other factors like clinical care.
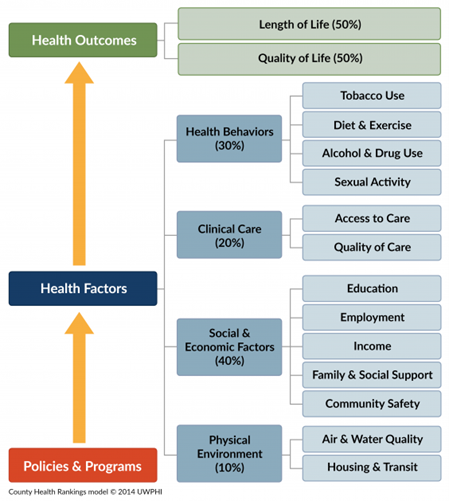
Social factors like homelessness and criminal justice involvement are often referred to as social determinants of health (SDOH). According to the Centers for Disease Control (CDC), “Social determinants of health (SDOH) are non-medical factors that influence health outcomes. They are the conditions in which people are born, grow, work, live, and age and the wider set of forces and systems shaping the conditions of daily life.” Everyone has social determinants of health that factor into their overall well-being, but not everyone is born with the same privileges or advantages.
SDOH and their distribution across our community are impacted by structural racism. Structural racism defined by the American Medical Association (AMA) “refers to the totality of ways in which societies foster racial discrimination through mutually reinforcing systems of housing, education, employment, earnings, benefits, credit, media, health care and criminal justice.” It has hugely shaped the distribution of privilege or disadvantage across the U.S., the ramifications of which stretch across multiple generations. Disadvantage, in a social construct, has paved the way for stigmatization; stigma can negatively impact opportunities and resources to achieve equitable health for some.
They start a trickle-down effect on SDOH. Jessica Jeruzal, MS, Operations Director at the HHCJ Lab explains, “If you imagine… social context, structural racism and stigma are [the] really big umbrella. And then that umbrella impacts the social determinants of health. And then further within that is your individual health and health outcomes.
At HHRI, we have a unique opportunity to interact with HHS patients many of whom have faced various impacts to their health from SDOH, structural racism, and stigma. We welcome the opportunity to think together with partners within and outside our systems about how we can all do better to consider and adapt our research and healthcare delivery processes to better support participation for all regardless of what privileges or disadvantages they were born into.
Fellow HHCJ team member, Senior Community Engaged Research Coordinator, Moncies Franco is no stranger to being impacted by SDOH. Growing up, Franco had low access to care and utilized the emergency room whenever he was sick because that’s what was passed down from generation to generation. Navigating the complexities of healthcare and traditional models of care wasn’t his area of expertise.
To exacerbate things further, Franco himself was impacted by the very stigma that he teaches about now. In 2010, his doctor insensitively and non-compassionately informed him, “You probably expected this, [but] you’re HIV positive.”
“And in that moment, what did I probably expect? Because that was the last thing that I was expecting at that moment. [This news] coming from a healthcare provider, really, it hurt in a way that I didn’t understand. It did escalate me into wanting to become involved in health care. And my story is one story, but it’s also a thread in the narrative of a lot of other stories that I hear from people who are impacted by social determinants of health.”
While it was difficult in that moment to be dealt such a devasting blow, Franco has been able to turn his pain into his purpose. “But I will say, from that moment, I’ve been able to heal and have a different outlook on life. I’ve also been able to use that moment as an educational moment for other providers, …and working at HHCJ Lab, I’ve gotten opportunities to speak with different residents and healthcare institutions and universities.
Personal stories have the power to change hearts and minds. And I think that when I retell that story to certain audiences, they understand, and hopefully there’s somebody in the audience who will consider. Consider what they say to the next person. And so, it’s an educational moment.
- Transitions Clinic Network: Post-Incarceration Addiction Treatment, Healthcare, and Social Support (TCN-PATHS)
- HHCJ is one of six sites participating in TCN-PATHS, a nationwide study led by Yale University exploring how to prevent opioid overdose for recently released inmates by utilizing transitional clinics versus traditional primary care clinics. The clinics are supported by community health workers who have lived experience as incarcerated individuals.
- Diabetes Homelessness Medication Support (DHOMES) and DHOMES Spanish
- Led by HHCJ Co-Director and internal family medicine practitioner, Dr. Kate Diaz Vickery, the D-HOMES study centers on folks living with Type 2 diabetes mellitus (T2DM) amongst people experiencing homelessness. They provide wellness coaching for ten weeks to improve participants’ medication adherence and provide community resources to improve health outcomes overall.
- Hennepin County Substance Use Disorder (SUD) Data Project
- Led by HHCJ Co-Director, Dr. Tyler Winkelman, the Hennepin County SUD data project is a partnership with HHCJ Lab, the MN Electronic Health Records Consortium, and Hennepin County. The group works to provide timely information about trends in substance-related healthcare patterns in order to inform prevention and response programs in our community.

Jeruzal and Franco recently brought their expertise to the Leadership Twin Cities, a program within the Minneapolis Regional Chamber for individuals seeking to build their understanding of the Twin Cities community’s greatest challenges and build the capacity to influence systemic change. The two gave a presentation on social determinants of health and shared how the HHCJ Lab’s work and research aims to get under the hood of SDOH by examining mental and physical health, substance use conditions, and the overlapping systematic barriers to health, through projects such as: